
A Day in the Life: Meet Martha, a Para Social Worker in Uganda

Para social workers (PSWs) play a critical role in strengthening community resilience for the protection of orphans and vulnerable children (OVC), particularly those living with HIV. PSWs act as a link between the clinic and the community, working to improve treatment outcomes.
Martha, pictured above, is a para social worker with Masaka Diocesan Medical Services (MDMS), a Bantwana implementing partner under USAID’s Integrated Child and Youth Development (ICYD) Activity.

Martha lives just a few meters away from a clinic in southern Uganda where she arrives bright and early at 7:00 AM each day.
Due to her background and experience, Martha doubles as a facility-based Linkage Facilitator and community-based PSW for the ICYD Activity. She uses her skills and experience to help clients navigate multiple facility departments while also providing critical community follow up through home visits. She begins her day at the Antiretroviral Therapy (ART) clinic by registering clients, organizing client files, updating the ART register, and booking new appointments.
“My husband abandoned me when I was pregnant,” explains Martha. “So I understand what women and children go through. That’s why I work hard to support them and ensure that they are protected and living fulfilling lives.”

After attending to all the clients, Martha calls those who have missed their appointments and reschedules them. She records the responses from the calls and shares the feedback with the PSW team for follow-up.
“The most common reasons for missed appointments are a lack of transportation to the facility, inadequate documentation, self-transfer, or migration,” says Martha.
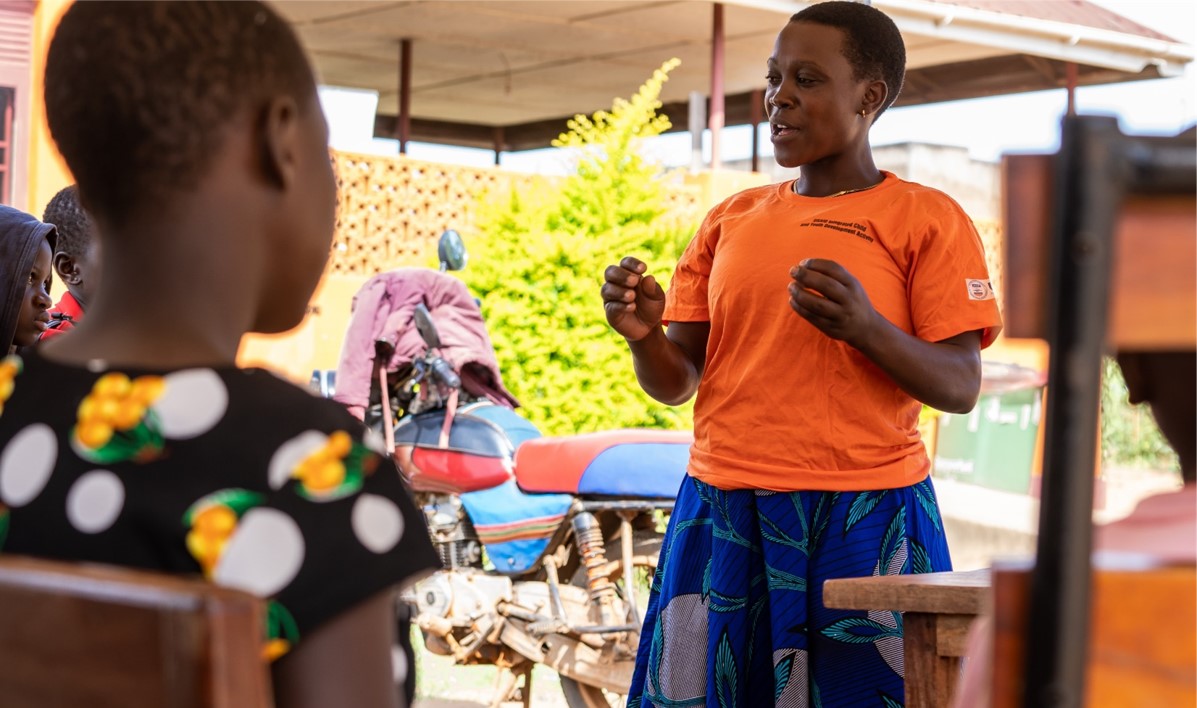
In the clinic’s waiting areas, Martha educates clients on various issues, including nutrition, treatment adherence, drug abuse, and viral load suppression.
She also provides growth and development sessions for children enrolled under the YAPS (Young Adolescent Programme Support) clubs, which help build social assets and agency.
“To ensure that clients receive the help they need, we refer them to other community-based organizations that provide services not provided by ICYD,” says Martha.
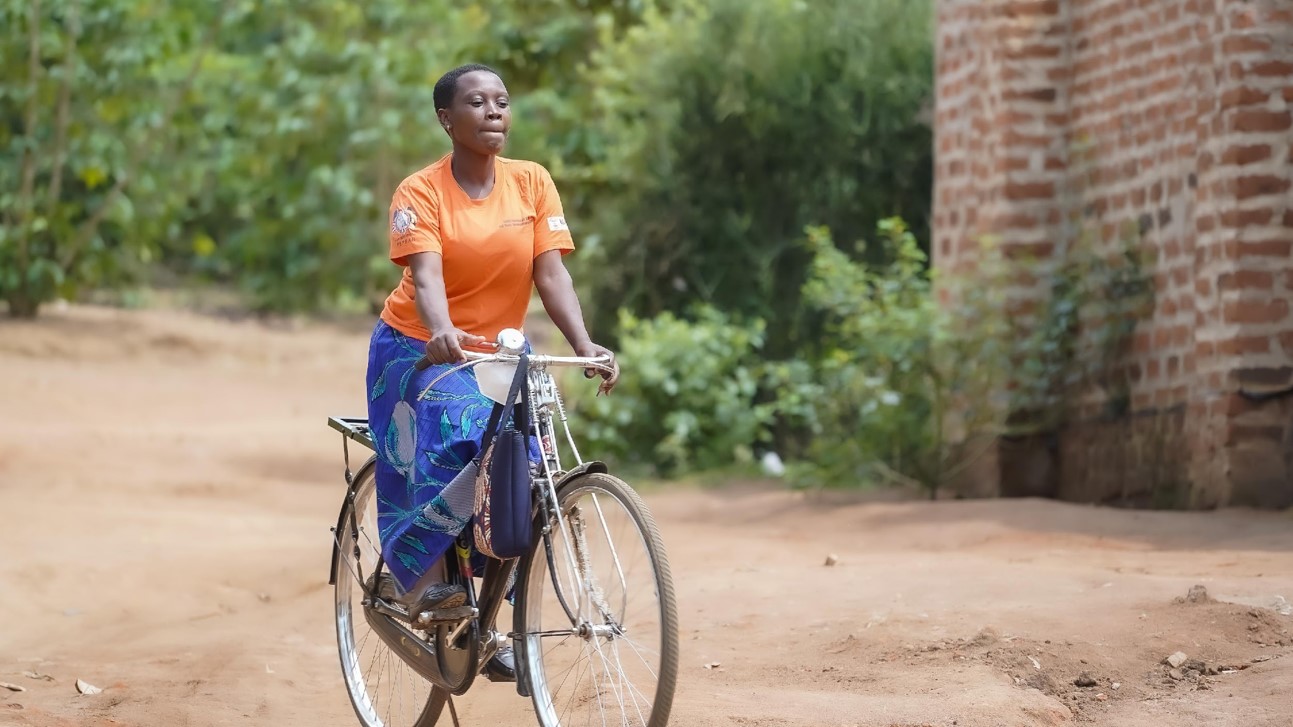
At 2:00 PM, Martha leaves the clinic to conduct home visits. On an average day she bikes over 6 miles and visits at least two households. Her PSW caseload is 25 households, and she visits each at least once a month.
Martha begins by first visiting those who need immediate care, including those who are non-suppressed and malnourished children.
![]() HIV medicine reduces the amount of HIV in the body (aka. viral load), which allows the immune system to keep working. This is called viral suppression.
HIV medicine reduces the amount of HIV in the body (aka. viral load), which allows the immune system to keep working. This is called viral suppression.
“Unlike my peers, I began riding a bicycle at a young age because I come from a farming family with only girls,” she explains.

Martha conducts cooking demonstrations during home visits to reinforce what is taught during teen and institutional support group sessions conducted at the health facility. Women are trained to prepare nutritious porridge among other meals in order to help their families maintain a balanced diet, boost immunity, avoid illness, and practice cleanliness and sanitation.
“We train beneficiaries to grow enough food for themselves and sell the surplus to purchase items they cannot produce at home,” she says.

An essential part of a home visit involves monitoring how and when medicine is taken and where it is stored. If the client or the caretaker has trouble remembering the time for medication, Martha sets an alarm on their phone or they discuss other types of reminders, such as favorite radio programs.
If the reason for poor drug adherence is more serious, such as refusal to take medication, Martha provides additional adherence counselling.
“To us, Martha is not just a para social worker, she is now a family member and has contributed to the healthy lifestyle we are living,” says a caretaker of one of Martha’s clients.

Poor drug adherence is the main cause of non-suppression and Martha, along with the other PSWs, spends a lot of time addressing these complexities.
“Sometimes the issue may not be medication but other cases like poor diet, gender-based violence, emotional abuse, isolation, and suicidal thoughts,” says Martha.

Martha then visits the rest of her clients to assess other types of health risks, such as poor diet, stress, inadequate hygiene, or lack of mosquito nets.
Once these risks are detected, they are addressed as soon as possible.

Finally, Martha records data on all the households she has visited that day.
At around 6:00 PM, after a hard day’s work, she returns home to get some much needed rest before starting again the next day.
